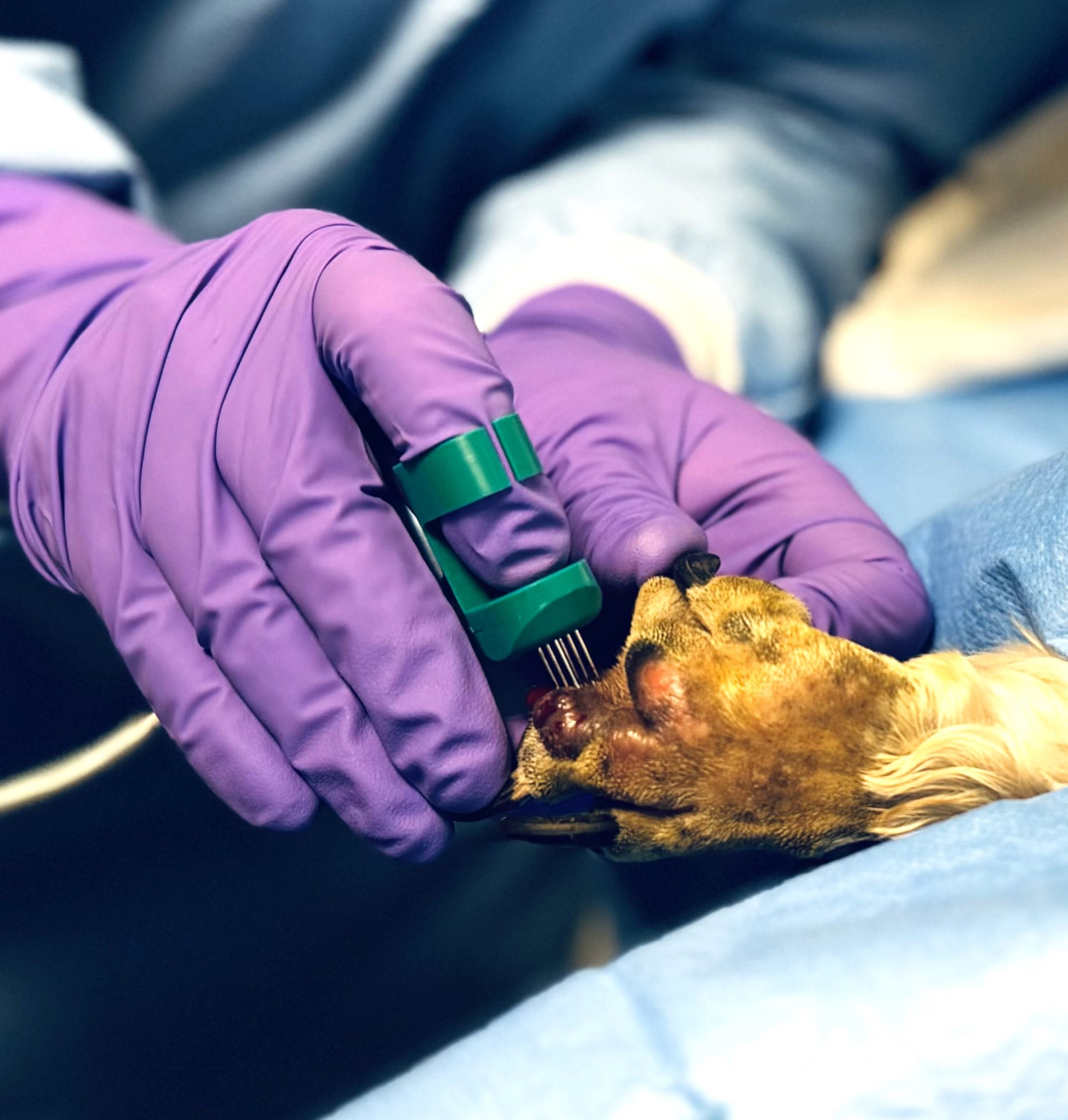
At Bridge Referrals, we are always investing and expanding the hospital services that we can offer the patients that are referred to us. In September of 2023 we introduced an additional treatment modality to our oncology department, called Electrochemotherapy. This made us one of only a handful of centres in the UK to offer this and the first in the North East!
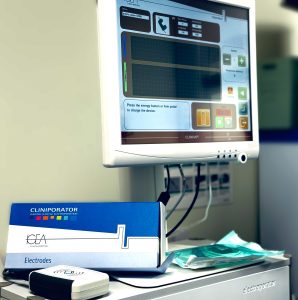
Electrochemotherapy unit at Bridge Referrals
What is electrochemotherapy?
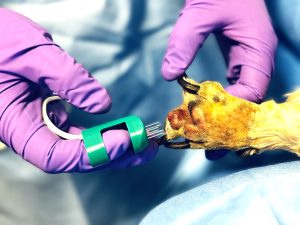
Poppy – The first Electrochemotherapy patient at Bridge Referrals
Electrochemotherapy (ECT) is a treatment aimed at localised cancers that combines chemotherapy and electric pulses that can amplify the local anti-tumour effect of the chemotherapy drug as well as being immunostimulant.
This consists of short (millisecond) high voltage pulses emitted by the electrical pulse generator. When a pulse reaches a cancer cell, the cell membrane opens up pores in the surface which allows the chemotherapy drug to diffuse into the cell. The drug is administered shortly before the procedure either intravenously or directly into the tumour itself.
Two primary cytotoxic agents can be used in electrochemotherapy which are Bleomycin and Cisplatin.
- Bleomycin is an anti-tumour antibiotic which, in normal situations, does not easily enter cells but can be very toxic once it is bound to the cancer cells DNA. When an electrical impulse is applied to the cell, Bleomycins efficacy increases by as much as 1000-fold.
- Cisplatin is another drug and is used only in dogs. It is a chemotherapy drug that contains Platinum and also has difficulty trying to enter cancer cells and is, again, highly toxic when binding to DNA. The use of electroporation increases the efficacy in cells by at least 80-fold
How can it help?
There are various ways that ECT can affect a cancer cell.
One effect is the enhanced cellular uptake of the chemotherapy drug by the cancer cells within the electric field.
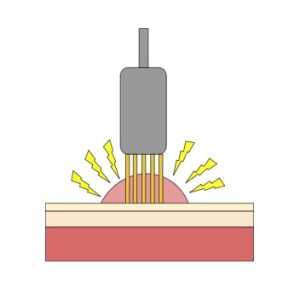
Diagram showing the insertion of needle electrodes into a tumour bed and pore formation at the cell membrane surface.
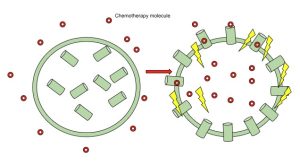
Another effect is the local constriction of blood vessels in the tumour bed. This is called a vascular lock and temporarily reduces blood flow to the cancer cells causing prolonged chemotherapy presence in the local area and starving the tumour bed of essential nutrients.
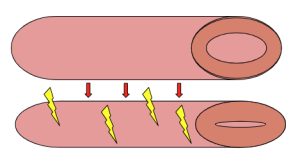
Vasoconstriction
Another mechanism is the activation of the immune system. When cells die, they release tumour antigens which may be recognised by the immune system inducing a form of immunity.
These mechanisms suggest that, regardless of tumour type or location, many tumours, regardless of type, should experience some degree of anti-tumour effect of ECT.
How soon after injection of a drug do we apply the electrical impulses?
If we are injecting directly into the tumour, then the impulses can be applied immediately. When the drug is injected into a vein, we must give the drug enough time to diffuse into the tumour tissue. This is usually between 5-8 minutes. The drug will remain at peak concentrations for approximately 20-40 minutes. If time between chemotherapy and impulses is delayed then the effectiveness will fall over time.
Are there any side-effects?
Given the reduced doses used in these patients, systemic side effects are not very common. All of this happens when the patients are under anaesthetic so no pain will be felt during the procedure. Sometimes, some local irritation may be seen which is treated with anti-inflammatory medications. Some transient reddening, oedema and possible tumour breakdown may be seen.
How many treatments are needed?
Most patients only need one to three treatments and each treatment lasts around 20-30 minutes oftem with 2-4 weeks between treatments depending on tumour response. Around 80% of patients will have variable degrees of response. The number of treatments needed is based on the response of the tumour as well as the size of the lesion to be treated.
When is it indicated?
Various tumours can benefit from the use of ECT. This can include squamous cell carcinoma, soft tissue sarcoma, mast cell tumour, localised lymphoma, melanoma, transmissible venereal tumours and anal sac adenocarcinoma.
ECT can be used in incompletely excised tumours or those that cannot be excised without significant complications to the patient. It can also be useful in cases in which radiation can either not be performed for various reasons.
Bridge Referrals first in the North East for Electrochemotherapy